At its core, the difference between an EMR and an EHR is all about scope. An Electronic Medical Record (EMR) is the digital equivalent of a patient's paper chart from one specific practice. In contrast, an Electronic Health Record (EHR) is a comprehensive, shareable health history that follows a patient wherever they go, from their primary doctor to a specialist to the hospital.
Think of an EMR as a digital filing cabinet for your office. An EHR, on the other hand, is more like a collaborative, lifelong health story.
Decoding EMR and EHR Systems
For any practice leader trying to fine-tune clinical workflows and improve patient care, getting the distinction between an EMR and an EHR right is essential. People often use the terms interchangeably, but they were designed to do very different things.
An EMR is really just a digital substitute for old-school paper charts. Its main job is to help with diagnosis and treatment within a single clinical setting. It's built to make things more efficient and organized inside the walls of your practice.
An EHR was created with a much bigger picture in mind. It gathers information from every clinician involved in a patient's journey and is built for interoperability. This means an EHR can securely share information with other providers—labs, specialists, hospitals, you name it—no matter where they are or what system they use.
The real takeaway is this: An EMR holds the medical and treatment history of patients within one practice. An EHR is designed to move with the patient, creating a complete health narrative that authorized providers can access across the entire healthcare landscape.
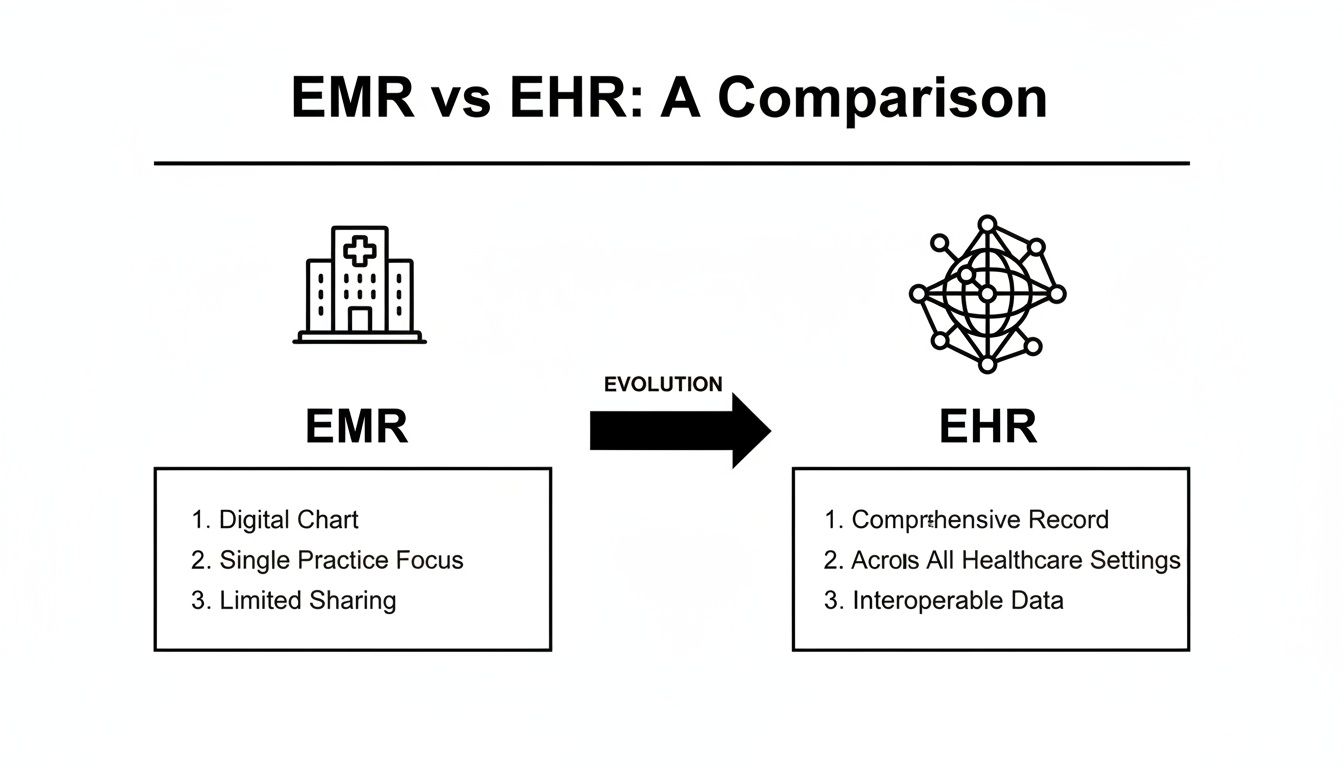
This visual gives a great breakdown of the EMR's single-practice bubble versus the EHR's interconnected approach.
As you can see, the EMR is an isolated system. The EHR acts as the central hub in a connected healthcare network.
Key Differences at a Glance
The move from paper to digital has been dramatic. Back in 2008, a mere 17% of office-based physicians were using any kind of EMR or EHR. Fast forward to 2014, and thanks to initiatives like the HITECH Act, certified EHR adoption jumped to 74% for physicians and 97% for hospitals. This rapid shift underscores the industry's push toward more connected, collaborative systems. You can dig into the full CDC data on adoption trends to see the whole story.
To really nail down the practical differences, it helps to see them side-by-side. This table breaks down their core characteristics.
Key Differences Between EMR and EHR Systems
| Characteristic | Electronic Medical Record (EMR) | Electronic Health Record (EHR) |
|---|---|---|
| Data Scope | Contains patient data from a single practice or organization. | Holds comprehensive patient data from multiple providers. |
| Interoperability | Limited; not built to be shared outside the individual practice. | High; designed for seamless data exchange across different systems. |
| Patient Access | Patients generally cannot access their own EMR directly. | Often includes a patient portal for accessing records and results. |
| Primary Use | Used for internal office management, diagnosis, and tracking treatment. | Built for coordinated care, patient-centered management, and clinical decision support. |
In short, while both systems digitize patient information, their purpose and reach are fundamentally different. An EMR looks inward, focusing on a single practice's needs, while an EHR looks outward, connecting the dots of a patient's entire healthcare journey.
A Closer Look at Functionality and Scope
When you get past the basic definitions, the real differences between EMR and EHR systems pop up in their core functions and overall scope. Think of an EMR as an internal tool, built from the ground up to replace paper charts and make a single practice run smoother. Its entire world exists within the four walls of your clinic.
An EMR is great at tasks like tracking patient data over time, flagging who's due for a check-up, or keeping an eye on vitals like blood pressure. It's a digital version of the old manila folder, streamlining diagnosis, treatment, and billing for one specific office. The system is designed, quite intentionally, to be self-contained.
This inward focus is also its biggest limitation. The moment a patient's information needs to go somewhere else—to a specialist, a lab, or a hospital—the EMR's usefulness drops off a cliff. You're often back to printing, faxing, or having staff manually re-enter data, which is exactly the kind of busywork you were trying to eliminate.
The Bigger Picture: EHR Functionality
An EHR, on the other hand, is designed with a much bigger picture in mind: a complete, long-term view of a patient’s health. It isn't just a digital chart; it’s a shared health dashboard that connects all the different players in the healthcare ecosystem. Its capabilities stretch far beyond a single practice.
An EHR is built to pull in and make sense of information from every stop on a patient’s care journey. This includes data from:
- Laboratories: Blood work and pathology reports flow directly into the patient's chart.
- Specialists: A cardiologist can instantly see the full history documented by the patient's primary care physician.
- Hospitals & ERs: Critical information, like allergies or current medications, is available when it matters most.
- Pharmacies: Prescription histories are tracked, helping to flag potential drug interactions.
This ability to aggregate data from multiple sources enables features that a standard EMR just can't offer. For example, an EHR can build a longitudinal patient record—a comprehensive, chronological story of a patient's health that all authorized providers can access. When you look at the different EMR systems on the market, you'll see their architecture simply isn't set up for this level of deep integration.
Here’s the bottom line: an EMR manages a patient’s record inside one practice. An EHR manages a patient’s overall health across the entire healthcare system. This is the fundamental split that makes EHRs so vital for coordinated, modern care.
Powering Advanced Clinical Work and Population Health
The wide-angle view of an EHR also unlocks tools that are becoming essential in healthcare. Clinical Decision Support (CDS) tools, for example, can analyze data from multiple sources to give clinicians real-time prompts. It might be an alert about an allergy to a medication prescribed by another doctor or a suggestion for a lab test based on recent results from an outside clinic.
EHRs are also the backbone of population health management. By gathering de-identified patient data across a network, organizations can spot health trends, track disease outbreaks, or measure how well public health campaigns are working. An EMR, with its data stuck in a silo, can't play a meaningful role in that larger mission.
Imagine a patient with diabetes.
- With an EMR: Their primary care doctor tracks blood sugar and prescriptions in one system. When they visit an endocrinologist, that specialist creates a brand-new, separate record. The podiatrist does the same. No one has the full story.
- With an EHR: The primary doctor, endocrinologist, and podiatrist all access and contribute to the exact same record. The system gives everyone a unified view of labs, treatments, and medications, ensuring every decision is based on complete information.
This collaborative power is what truly sets them apart. It shows why the EMR vs. EHR debate isn't just about technology—it has a direct and profound impact on the quality and safety of patient care.
Understanding Interoperability: The Critical Dividing Line
When we talk about EMRs and EHRs, the discussion often circles back to one core concept: interoperability. This isn't just a technical buzzword; it's the fundamental difference that defines how these systems function and, ultimately, how they impact patient care. Think of it as the difference between a locked diary and a shared, collaborative patient story.
An Electronic Medical Record (EMR) is, by its very nature, a closed loop. All the rich patient data it holds—diagnoses, treatments, medications—is essentially confined to the four walls of your practice. This creates digital silos, making it incredibly difficult to share information with anyone outside your organization.
What happens when a patient needs a referral to a specialist or is admitted to the hospital? With an EMR, you’re often thrown back into the dark ages of healthcare communication. Staff end up printing out piles of records, wrestling with fax machines, or manually keying in data from one system to another. It’s a huge administrative headache and a recipe for human error.
The EHR Approach to Data Exchange
On the other hand, Electronic Health Records (EHRs) were built with data sharing in mind. They are designed to communicate securely with other systems, adhering to national standards like Health Level Seven (HL7) that act as a universal language for healthcare information. This allows systems from completely different vendors to talk to each other.
This connectivity is what allows an EHR to build a comprehensive health story that follows the patient wherever they go. It's not just a snapshot of what happened in your office; it’s the full narrative of their entire healthcare journey. This has a massive impact on daily clinical life.
The design of the system directly correlates to how much time your team spends bogged down in administrative work. The numbers don't lie. US doctors spend a median of 90.1 minutes per day in their systems, a staggering 31.8 minutes more than their non-US peers. A siloed EMR contributes heavily to this, forcing redundant data entry every time a patient sees a new provider. You can dig into the full research published in JAMA to see just how deep this problem runs.
Interoperability isn’t just a feature. It’s the engine that turns a static record into a dynamic tool for coordinated care. It’s what ensures a patient's information is in the right place, at the right time, for the right provider.
A Patient Journey: EMR vs. EHR
Let’s walk through a real-world scenario to see how this plays out. A patient goes from their primary care physician to a specialist and then to the hospital.
Scenario with an EMR:
- Primary Care: The patient sees their family doctor for chronic joint pain. The visit is documented in the clinic’s EMR, and a referral is made to a rheumatologist.
- Specialist Visit: The rheumatologist’s office calls to request records. The primary care team faxes over a thick stack of papers. Someone at the specialist's office then has to manually scan or re-enter this data into their own EMR.
- Hospitalization: The patient has a severe flare-up and ends up in the ER. The hospital staff has no immediate access to the patient's history from either the primary doctor or the specialist, leading to potential care delays and redundant, costly tests.
Scenario with an EHR:
- Primary Care: The doctor documents the visit in their EHR and sends a digital referral directly to the rheumatologist.
- Specialist Visit: The rheumatologist’s team securely accesses the patient's shared record through the EHR network. They see the primary doctor's notes, lab results, and medication list in real-time—before the patient even walks in the door.
- Hospitalization: At the ER, the attending physician pulls up the patient’s complete, longitudinal health record. They can instantly see diagnoses, allergies, and medications from all previous providers, enabling them to make faster, safer, and more informed treatment decisions. To make this work, you need the right infrastructure, which is why choosing the right medical practice IT support is so critical.
The difference is night and day. An EMR-based workflow is fragmented, inefficient, and puts a huge burden on both staff and patients. An EHR-powered workflow, however, is cohesive and collaborative, paving the way for better care coordination and genuinely better outcomes.
How Each System Impacts Daily Clinical Workflows
The real-world differences between an Electronic Medical Record (EMR) and an Electronic Health Record (EHR) show up in the day-to-day grind of a clinical practice. While both are a massive leap from paper charts, their effects on workflow, decision-making, and your staff's administrative load are worlds apart. Think of an EMR as a digital filing cabinet—great for what's inside, but isolated from everything else.
Picture this common scenario: a clinician is trying to diagnose a patient, but they’re working with incomplete information. They need recent lab results from another facility to confirm a suspicion, but the EMR can't pull that data. The entire workflow screeches to a halt. Staff members are now stuck making phone calls and sending faxes, which delays the diagnosis and piles on administrative work.
This isn't a rare occurrence in practices that rely on EMRs. The system is built for internal record-keeping, not for collaboration with the outside world. This forces your team into manual workarounds that drain time, energy, and introduce the potential for human error.
The EMR Workflow: A Series of Hurdles
In a practice running on an EMR, the clinical workflow often feels disjointed. This is especially true for patients with complex health needs who see multiple providers. Every time that patient steps outside your practice, another data silo is created.
Here’s a look at how an EMR workflow typically breaks down:
- Manual Data Reconciliation: A new patient comes in from another clinic, and your staff has to manually type in their entire history, medication list, and allergies. It’s tedious and a perfect recipe for transcription errors.
- Delayed Clinical Decisions: Your primary care physician refers a patient to a specialist. But without shared records, the specialist is starting from scratch, often leading to repeated tests and a slower path to a treatment plan.
- Inefficient Communication: Need to share a patient's chart? You're back to printing, scanning, or faxing. This administrative drag pulls your clinical team away from what they should be doing—caring for patients.
These bottlenecks are more than just frustrating; they carry real financial and clinical weight. The gap between the two systems is stark, as EHRs are designed to support the kind of collaboration that drives better reimbursements and outcomes. In fact, practices sticking with older EMRs can miss out on full Medicare and Medicaid reimbursements, since only certified EHRs have qualified under Meaningful Use rules since 2011.
This reality helps explain the massive shift in the industry: hospital EHR adoption jumped from just 9% in 2008 to 96% by 2014, while physician adoption climbed from 17% to 78%. For a closer look, you can explore the full breakdown of the EMR-EHR financial gap.
The EHR Workflow: A Cohesive Patient Story
An EHR fundamentally changes the game by putting a complete, up-to-the-minute patient history right in the provider's hands. Clinicians can stop chasing down information and start focusing on making informed decisions at the point of care.
With an EHR, the workflow shifts from reactive data gathering to proactive clinical management. It empowers providers by presenting a unified health narrative, reducing medical errors and enabling more effective treatment strategies.
An EHR-powered workflow makes an immediate impact on daily operations:
- Automated Information Exchange: Lab results, notes from a specialist, and hospital discharge summaries flow directly and securely into the patient’s record. No more manual entry.
- Enhanced Patient Safety: The system can automatically flag potential drug interactions by checking prescriptions from multiple doctors—a safety net that a siloed EMR simply can't provide.
- Streamlined Referrals: A primary care doctor can send a digital referral that includes the patient’s entire history, ensuring the specialist has all the context they need before the appointment even starts.
This cohesive approach doesn't just improve the quality of care; it also slashes the administrative burden on your staff. They can finally dedicate more time to high-value tasks and patient engagement. When you see it in action, the difference is clear: one system creates friction, while the other creates flow.
Choosing The Right System For Your Practice
Deciding between an EMR and an EHR really boils down to your practice's specific needs, your long-term goals, and how you approach patient care. This isn't just about picking software features; it's about what makes sense for your daily workflow. While a basic EMR might seem like enough for some clinics, most modern practices find that a true EHR is the only way to support growth and deliver high-quality, coordinated care.
Different types of practices have completely different demands. What works for a solo practitioner's office is unlikely to support the complex, collaborative needs of a multi-specialty group. Understanding the practical difference between an EMR and an EHR in these real-world settings is the key to making a smart investment.
For Medical Spas and Aesthetic Practices
Medical spas are a unique blend of healthcare and hospitality. They juggle complex treatment packages, memberships, and detailed client histories. An EMR can certainly track individual procedures, but it often misses the bigger picture—the client's overall health context, which is critical for ensuring safe and effective aesthetic treatments.
This is where an integrated EHR becomes non-negotiable. It gives practitioners a place to document crucial health information, like allergies or medications prescribed by a primary care doctor, that could directly impact an aesthetic procedure. It’s about creating a safer experience for the client and having the ability to communicate with their broader care team if something comes up.
For Primary Care and Wellness Clinics
Think of primary care as the quarterback of the healthcare system. These clinics are the central hub, coordinating care across a wide network of specialists, managing chronic conditions, and focusing on a patient's long-term wellness. An EMR, with its siloed data, just creates roadblocks to that mission.
For a primary care practice, an EHR isn't just a nice-to-have; it's essential. The interoperability it provides is what allows you to share records with cardiologists, endocrinologists, and hospitals in real-time. This ensures every provider involved has a complete view of the patient's health, which is fundamental for better chronic disease management and preventive care.
The right system isn't just about digitizing records; it's about building a technology foundation that mirrors your care delivery model. For collaborative, patient-centered practices, an EHR is the only path forward.
For Specialty and Concierge Practices
High-touch specialty and concierge practices stake their reputation on delivering a superior, deeply personalized patient experience. Their clients don't just expect good care; they expect proactive, seamless coordination and a provider who understands their unique health story inside and out. A simple EMR just can’t provide the 360-degree view needed for that level of service.
A powerful EHR is fundamental to elevating the patient journey in these high-value settings. It gives clinicians a complete, longitudinal view of a patient’s health by pulling in data from all of their other providers. This is what allows for truly personalized health plans, proactive follow-ups, and the kind of white-glove service that justifies a premium model.
Ultimately, your choice depends on your vision for patient care. If your practice truly operates in a silo, an EMR might get the job done. But if you see yourself as an active, collaborative part of a patient's total health journey, an EHR is the only logical choice. To explore this further, take a look at our guide on finding the best EMR for a private practice, which digs into these factors in more detail.
Moving Beyond Standalone EHRs to Integrated Platforms
Choosing an EHR over a more limited EMR is a solid move for any practice. But even the best EHR can create new headaches if it's working all by itself. Modern practices are juggling a whole tech stack—scheduling, billing, patient portals, marketing tools—and this often leads to what we call the "8-12 vendor problem."
When you have that many separate systems, each one becomes its own little island of data. Your team ends up wasting time copying and pasting information from one platform to another. It’s more than just a time-waster; this manual shuffle opens the door to security risks and expensive data entry mistakes. The real issue is that these standalone tools were never built to talk to each other, leaving you with a tech setup that feels disjointed and clumsy.
The Rise of the Vertically Integrated Ecosystem
The way out of this vendor mess is a vertically integrated platform. In this setup, the EHR isn't a separate piece of software you buy. Instead, it's a native, core part of one single, unified system that handles everything. This goes way beyond the typical "integrations" that often break or need constant upkeep. We're talking about a genuinely seamless environment where data moves freely between every part of your practice.
Think about it: a patient books an appointment online, and that single action instantly updates the schedule, creates a chart in the EHR, and preps the billing module. No one on your team has to lift a finger. That's what vertical integration delivers. It kills redundant data entry and guarantees everyone is working from the same real-time information.
When the EHR becomes a central piece of a purpose-built platform, you get rid of data silos, tighten up security, and build workflows that just work. Your technology stops being a jumble of tools and starts being a real strategic asset.
Unlocking True Operational Efficiency
This unified approach gives you a massive advantage over just buying a standalone EHR. When every tool—from the first time a patient contacts you to their final payment—lives in the same ecosystem, your whole operation becomes more secure, compliant, and efficient. Data isn’t locked away in different programs anymore; it’s a shared resource that helps you make smarter clinical and business decisions.
The benefits are real and you'll feel them quickly:
- Smoother Workflows: Your staff can stop wasting their day switching between different logins and manually checking if the data matches up.
- Tighter Security: A single, secure platform has far fewer weak points for cyber threats than trying to manage security across a dozen different vendors.
- A Better Patient Experience: Patients get a smooth, consistent journey, from booking to follow-up, with easy access to their information.
The next step in modernizing your practice isn't just about picking an EHR vendor; it's about finding a true technology partner. If you're weighing your options, getting familiar with what modern healthcare practice management software can do is key to building a practice that's connected and built to last. It's the difference between simply going digital and truly optimizing your entire business.
Frequently Asked Questions
When you're running a practice, the EMR vs. EHR debate isn't just theoretical. It brings up very real, practical questions about cost, security, and what to do with the system you already have. Getting the definitions right is the first step, but the follow-up concerns are what truly shape your decision.
Let's dig into some of the most common questions we hear from practice owners weighing their options.
Can You Upgrade an EMR to an EHR?
This question comes up all the time, but the answer is nearly always no. You can't just "upgrade" an EMR to an EHR in the way you'd update an app on your phone. Their core designs are just too different. An EMR is built to be a closed loop—a digital version of a paper chart for one office.
An EHR, on the other hand, is built from the ground up to connect and share information securely with other providers, labs, and pharmacies. So, moving from an EMR to an EHR isn’t an upgrade; it’s a full system replacement and data migration. You're fundamentally switching to a new platform designed for connectivity.
Are EHR Systems More Expensive Than EMRs?
At first glance, an EMR might seem like the cheaper option because its scope is so much smaller. But that initial price tag doesn't tell the whole story. You have to look at the Total Cost of Ownership (TCO). While an EHR might have a higher upfront cost, its long-term Return on Investment (ROI) is almost always better.
Think about the hidden costs of being stuck with a data silo like an EMR:
- Administrative Overhead: How much time does your staff spend on the phone, at the fax machine, or manually entering data from a specialist’s report? It adds up.
- Missed Reimbursements: Many government incentive programs are tied specifically to the use of certified EHRs.
- Clinical Inefficiencies: When a doctor can't easily access a patient's records from another clinic, it can lead to redundant tests and delays in care.
An EHR's value lies in its ability to streamline workflows and improve care coordination, generating long-term financial and clinical benefits that isolated EMRs cannot match.
What Are Key Security Concerns with EHR Data Sharing?
Naturally, the idea of sharing patient data brings security to the forefront. Being HIPAA compliant is the absolute baseline for any system you consider, but true security goes much deeper. It means end-to-end encryption for data, strict access controls that limit who can see what, and routine security audits to find and fix vulnerabilities.
One of the biggest security advantages of a unified platform is that it shrinks your attack surface. Trying to manage compliance and security across a dozen different software vendors is a nightmare. A single, integrated ecosystem gives you a more controlled and secure environment, making it far easier to protect patient data and stay compliant.
Stop juggling multiple vendors and unlock true operational excellence. Ragnar STACK provides a single, vertically integrated platform where your EHR, billing, and patient communications work together seamlessly. Discover a better way to run your practice at https://notes.rstack.io.